
Anouk Charlot, Université de Strasbourg and Joffrey Zoll, Université de Strasbourg
On top of kickstarting a new exercise regime, the new year is traditionally a period when many people reconsider their eating habits. In recent years, intermittent fasting has become a popular habit – and has been credited with some health benefits, be it to manage excess weight, chronic illnesses, or flagging energy levels. But what exactly is intermittent fasting? And does all the hype around it stand up to scientific scrutiny?
The term intermittent fasting covers several approaches, each based on different principles. It is important to note that no matter which method is used, the restrictions only affect food – never water – intake.
-
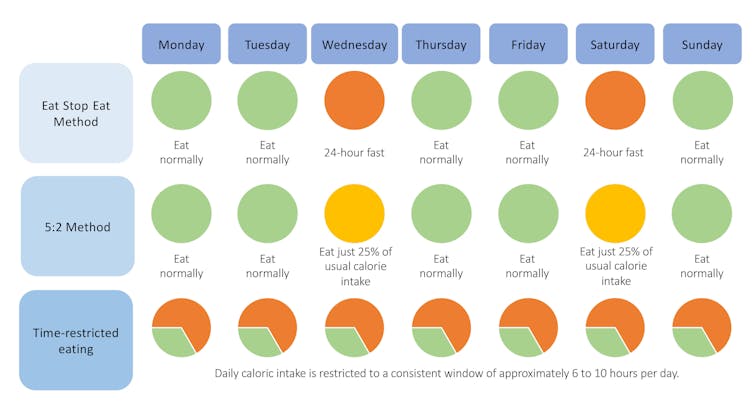
The “Eat Stop Eat” method. Put forward by Brad Pilon in his book of the same name; the principle is to alternate days of normal eating and fasting, including two non-consecutive fasting days in a week.
-
The 5:2 method. Developed in the 2000s by doctors Michelle Harvie and Tony Howell, this alternates between five days of normal eating and two days (which can be consecutive) of 70-75% calorie reduction during the week.
-
Time-restricted eating (also called time-restricted feeding). This is currently the most popular and studied method. It consists of narrowing the food intake window to between 6 and 10 hours per day and therefore fasting between 14 and 18 hours during the day.
Science’s verdict?
Outcomes vary depending on the adopted strategy.
With the “Eat Stop Eat” and 5:2 approaches, relatively few scientific studies have been conducted. The little available data have shown they can effectively help us lose weight and improve certain metabolic parameters such as fasting blood glucose. For example, the nutritionist Surabhi Bhutani showed the use of the 5:2 method for three months resulted in a weight loss of 3-6 kg in participants.
However, both methods are very restrictive and can cause side effects on days of total fasting or severe caloric restriction – hunger, negative effects on mood, and risk of hypoglycemia.
In the longer term, the restriction also increases the risk of developing or worsening eating disorders and yo-yo dieting. These patterns often appear after the individual has attempted to lose weight by restricting themselves. Despite initial progress, the deprivation is likely to generate frustrations that will encourage the return of old eating habits.
The most studied method is the one with a daily food intake but limited time. Two “time slots” are often observed:
-
When food intake starts with breakfast and ends in the late afternoon – known as “early time-restricted feeding.”
-
When food intake starts with lunch – known as “late time-restricted feeding.”
This approach appears to improve metabolic regulation and slash the risk of metabolic diseases. However, these benefits vary according to the chosen time slot. When food intake starts in the morning, studies have observed weight loss and improvements in insulin sensitivity.
Conversely, there are fewer or no benefits to starting meals at midday and ending them in the evening. Ram Babu Singh’s team (Halberg Hospital and Research Institute, India) also showed positive results in participants who ate only in the morning and not in those who ate in the evening after 8 p.m.
Why such a difference?
Research suggests our internal clock and circadian rhythms may have something to do with it. Indeed, the benefit of only eating in the morning is that the periods of food intake and fasting coincide with our biological clock.
In our previous article, we explained that in response to light cycles, our body produces hormones in a cyclical way to adapt our food intake to the body’s energy needs: the optimal period for eating is, therefore, from around 8 or 9 a.m. (when the sun rises) to 7 p.m. (when the sun starts to set, depending on the season).
Not eating breakfast and eating after 7 p.m. upsets circadian rhythms and increases the risk of developing metabolic diseases.
However, while time-limited eating seems to be a good approach to metabolic health, much remains to be understood about how it works and how to optimize its effects. Work in 2022 showed no difference in weight loss between opting for early- or late-morning eating. It did, however, affect appetite during the day – this time to the advantage of the former.
And beyond the time of day when it seems preferable to eat, other factors may be at work that is not always measured in the studies carried out: quality and quantity of food absorbed, duration of the fasting period (which can extend from 12 to 20 hours per day), etc. It is also worth remembering every individual has his or her metabolism and may respond differently to fasting. New, better-controlled, and more comprehensive studies are therefore needed to confirm these methods’ potential benefits and understand the mechanisms involved in their effects.
In practice, what to do?
The most suitable method to avoid disrupting one’s circadian clock (thereby limiting the risk of frustration or eating disorders) appears to be time-limited food intake by synchronizing meals with circadian rhythms.
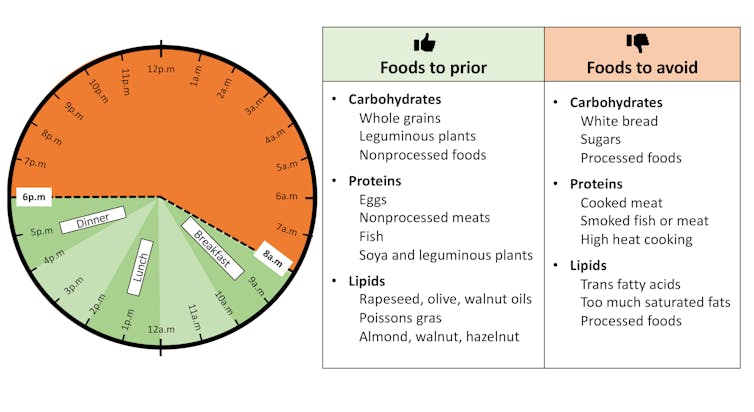
Thus, a typical day could be organized with a hearty breakfast between 6 and 8 a.m., lunch around midday, and finally bringing, dinner forward so that it takes place between 4 and 6 p.m., depending on the season.
This is not necessarily easy to reconcile with one’s social life. It can be complicated to practice intermittent fasting for a family when one practices a sporting activity in the early evening or works in the evening until 7 or 8 p.m.
One solution would be to opt for a big breakfast and not too caloric a meal in the evening – preferably without carbs or sugars, so as not to risk shifting one’s biological clock.
Anouk Charlot
Chrono-nutrition
Chrononutrition is increasingly popular, and intermittent fasting appears to boost metabolic health effectively. That said, we have seen it is not a panacea. And we must ensure that the periods of fasting and food intake are consistent with our biological clock.
In the face of many existing methods and potential risks, patients and health professionals still lack information. Further research is essential to understand their effects better. Currently, there is no consensus on the ideal time to eat/fast or the optimal duration of each period. Moreover, these parameters may differ from one person to another, depending on their genetic makeup, history, and lifestyle. Therefore, it is important to consider using this dietary strategy with qualified health professionals to set up a healthy and balanced diet that will limit the risk of complications.![]()
Anouk Charlot, Doctorante, Université de Strasbourg and Joffrey Zoll, MCU-PH en physiologie, faculté de médecine, Université de Strasbourg
This article is republished from The Conversation under a Creative Commons license. Read the original article.


16 Comments
Pingback: naza24
Pingback: สล็อตแตกง่ายสล็อตเว็บตรงสล็อตpg
Pingback: เดิมพันเกม Esports
Pingback: jarisakti
Pingback: เช่ารถตู้พร้อมคนขับ
Pingback: ประมวลรัษฎากร
Pingback: ผ้า
Pingback: namo333
Pingback: xxxโอลี่แฟน
Pingback: pakkumised ja teenused
Pingback: Jinda888 คืออะไร
Pingback: แกนกระดาษ
Pingback: ส่งพัสดุ
Pingback: slot onlineค่ายเกมดังยอดฮิต 2023
Pingback: kado bar 10000
Pingback: Nature’s Ozempic: What and how you eat can increase levels of GLP-1 without drugs - Bergensia