
Michael (Mike) Joy, Victoria University of Wellington et Michael Baker
Last year, a Danish study reported a link between nitrate in drinking water and the risk of developing colorectal (bowel) cancer. This finding could have important implications for New Zealanders.
New Zealand has one of the highest bowel cancer rates in the world. Recent data show also that drinking water supplies in some parts of New Zealand have nitrate levels more than three times higher than the threshold level for colorectal cancer risk identified in the Danish study.
This study and other research raise an important question about the contribution nitrate exposure through drinking water may be making to New Zealand’s high rates of bowel cancer.
À lire aussi :
What’s behind the increase in bowel cancer among younger Australians?
Health implications of nitrates in drinking water
Nitrate fertiliser is added to pasture and crops to accelerate plant growth. Much of it enters waterways either directly with rain and irrigation or through animal urine.
The Danish study, published in the International Journal of Cancer, was extensive both in number of participants and length of follow-up. It included 2.7 million people over 23 years and monitored their individual nitrate exposure levels and colorectal cancer rates.
The findings confirmed widely held suspicions that long-term exposure to nitrate may be linked to cancer risk. The investigators propose that the risk results from nitrate converting into a carcinogenic compound (N-nitroso) after ingestion.
The research found a statistically significant increase in colorectal cancer risk at 0.87ppm (parts per million) of nitrate-nitrogen in drinking water. There was a 15% increase in risk at levels over 2.1ppm, compared with those who have the least exposure.
One key implication is that the current nitrate standard for drinking water used in most countries, including New Zealand, is probably too high.
International nitrate standards
The cancer risk level (0.87ppm) identified in the study is less than a tenth of the current maximum allowable value (MAV) of nitrate-nitrogen of 11.3ppm (equivalent to 50ppm of nitrate). This level has been in use in many countries for decades and comes from the World Health Organisation’s limit. It is based on the risk of “blue baby syndrome” (infantile methaemoglobinaemia, a condition that reduces the ability of red blood cells to release oxygen to tissues) – but not the risk of cancer.
Rates of bowel cancer vary across New Zealand, with the highest incidence in South Canterbury, with an age-standardised rate of 86.5 cases per 100,000 people. Bowel cancer is the second-highest cause of cancer death in New Zealand and each year around 3,000 people are diagnosed and 1,200 die of the disease.
A recent epidemiological review estimated the contribution of a range of modifiable “lifestyle” risk factors to colorectal cancer in New Zealand. In order of importance, these factors are obesity, alcohol, physical inactivity, smoking and consumption of red meat and processed meat. It would be useful to conduct more research to see if nitrate exposure in drinking water should be added to this list.
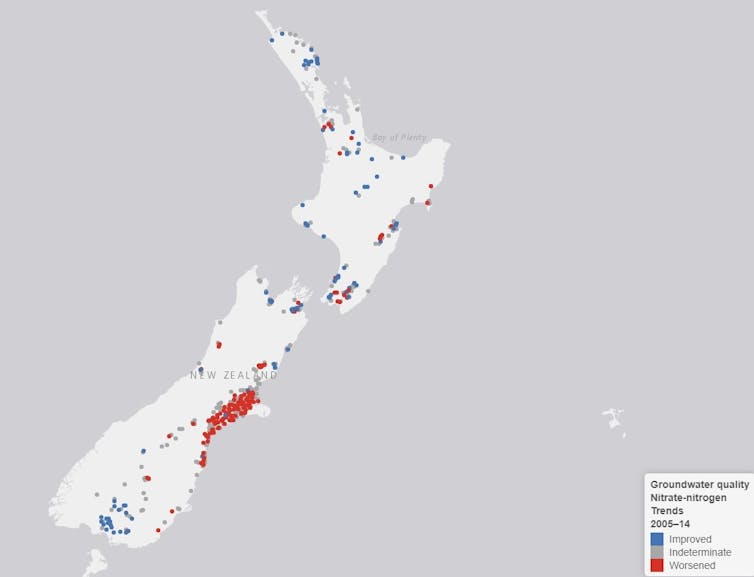
Ministry for the Environment, Stats NZ, CC BY-ND
A recent Fish and Game New Zealand investigation of drinking water supplies in the Canterbury region found that nitrate levels in drinking water sourced from groundwater in areas of intensive farming and horticulture are already high and rising. The findings are consistent with data from the regional council Environment Canterbury. The latest groundwater report showed that half of the wells they monitor have values greater than 3ppm nitrate-nitrogen, more than three times the Danish study’s trigger level for colorectal cancer risk.
Christchurch City Council data show that of 420 samples collected during five years from 2011 to 2016, 40% exceeded 0.87ppm.
À lire aussi :
You’ve heard of a carbon footprint – now it’s time to take steps to cut your nitrogen footprint
Impact on ecosystems
When nitrate enters waterways, it accelerates algae growth. Freshwater scientists have long been pushing for nitrate limits to curtail algal proliferation, but restrictions have been slow and in some regions non-existent. An important coincidence is that the Australian and New Zealand guideline for healthy aquatic ecosystems for nitrate is at 0.7mg/l nitrate-nitrogen, close to the level required to stay under the colorectal cancer risk value found in the Danish study.
The Canterbury region exemplifies the problems resulting from the failure of central and local government policy in New Zealand to protect both ground and surface water. These failures cannot be blamed on a lack of awareness as these outcomes were predicted decades ago. For example, in 1986 the Ministry of Works predicted the nitrate contamination we now see as a consequence of regional irrigation schemes. It made it clear that alternative drinking water supplies would have to be found for Canterbury residents.
Apart from health and ecological concerns, another worry is that public fears about drinking water safety will prove a boon for water bottling companies, which have free access to New Zealand’s cleanest water.
While many New Zealanders face significant and increasing costs for water treatment, water bottlers pay virtually nothing. The only cost, apart from bottling costs, is a one-off 35-year regional council consent fee. This anomaly highlights the urgent need for government to put tougher limits on nitrate loss and face up to dealing with water ownership issues in New Zealand.
In conclusion, surface water in many parts of New Zealand is highly contaminated with nitrates as a result of intensified farming. These elevated levels are undoubtedly damaging freshwater ecosystems and biodiversity, and may also be harming human health.
At the very least, public health authorities need to conduct a systematic survey to assess current nitrate levels in New Zealand drinking waters, including those that are not part of the routinely monitored networked system. This information could then be used to provide a quantitative estimate of the colorectal cancer burden in New Zealand that can be attributed to this hazard.![]()
Michael (Mike) Joy, Senior Researcher; Institute for Governance and Policy Studies, Victoria University of Wellington et Michael Baker, Professor of Public Health
Cet article est republié à partir de The Conversation sous licence Creative Commons. Lire l’article original.



8 Comments
Pingback: naga356
Pingback: รับทำเว็บไซต์
Pingback: more information
Pingback: ศูนย์ดูแลผู้สูงอายุ
Pingback: Buy Colt AR-15 Pistol Upper Receiver Assembly 5.56x45mm 14.5" Barrel, No Handguard Online At theblissfirearms.com
Pingback: carts for sale
Pingback: aroundtravel
Pingback: เว็บ slot รองรับทรูวอเล็ท