Michael Baker, University of Otago; Amanda Kvalsvig, University of Otago, and Nick Wilson, University of Otago
On Sunday, New Zealand will mark 100 days without community transmission of COVID-19.
From the first known case imported into New Zealand on February 26 to the last case of community transmission detected on May 1, elimination took 65 days.
New Zealand relied on three types of measures to get rid of the virus:
- ongoing border controls to stop COVID-19 from entering the country
- a lockdown and physical distancing to stop community transmission
- case-based controls using testing, contact tracing and quarantine.
Collectively, these measures have achieved low case numbers and deaths compared with high-income countries in Europe and North America that pursued a suppression strategy.
New Zealand is one of a small number of jurisdictions – including mainland China, Hong Kong, Taiwan, South Korea, Vietnam, Mongolia, Australia and Fiji – pursuing COVID-19 containment or elimination. Most have had new outbreaks. The exceptions are Taiwan, Fiji and New Zealand.
Australia adopted very similar responses to the pandemic and it is important to note that most states and territories are in the same position as New Zealand. But Victoria and, to a lesser extent, New South Wales are seeing a significant resurgence.
The key difference is that New Zealand committed relatively early to a clearly articulated elimination strategy and pursued it aggressively. An intense lockdown proved highly effective at rapidly extinguishing the virus.
This difference can be seen graphically in this stringency index published by Oxford University’s Our World in Data.
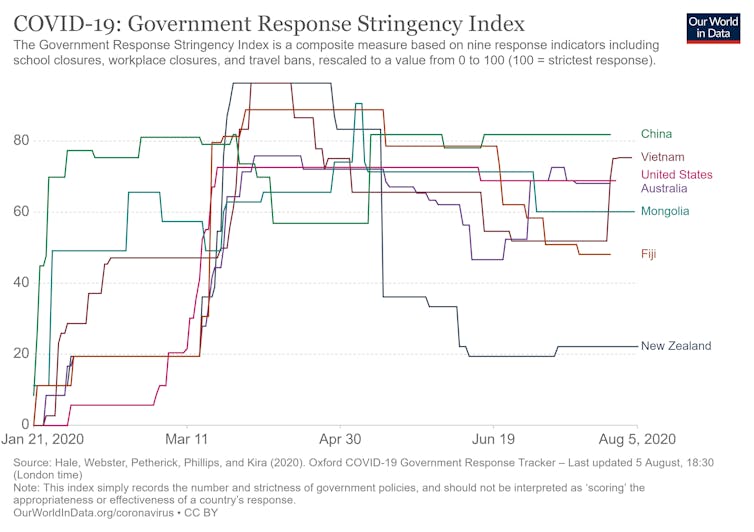
There are key lessons from New Zealand’s COVID-19 experience.
A vigorous, decisive response to the pandemic was highly effective at minimising cases and deaths. New Zealand has the lowest COVID-19 death rate in the OECD.
Total all-cause deaths also dropped during the lockdown. This observation suggests it did not have severe negative effects on health, although it will almost certainly have some negative long-term effects.
Elimination of the virus appears to have allowed New Zealand to return to near-normal operation fairly rapidly, minimised economic damage compared with Australia. But the economic impact is likely to keep playing out over the coming months.
Getting through the pandemic
We have gained a much better understanding of COVID-19 over the past eight months. Without effective control measures, it is likely to continue to spread globally for many months to years, ultimately infecting billions and killing millions. The proportion of infected people who die appears to be slightly below 1%.
The infection can cause serious long-term consequences for some people. The largest uncertainties involve immunity to this virus, whether it can develop from exposure to infection or vaccines, and if it is long-lasting. The potential for treatment with antivirals and other therapeutics is also still uncertain.
This knowledge reinforces the huge benefits of sustaining elimination. We know that if New Zealand were to experience widespread COVID-19 transmission, the impact on Māori and Pasifika populations could be catastrophic.
We have previously described critical measures to get us through this period, including the use of fabric face masks, improving contact tracing with suitable digital tools, applying a science-based approach to border management, and the need for a dedicated national public health agency.
Read more:
New Zealand hits zero active coronavirus cases. Here are 5 measures to keep it that way
Maintaining elimination depends on adopting a highly strategic approach to risk management. This approach involves choosing an optimal mix of interventions and using resources in the most efficient way to keep the risk of COVID-19 outbreaks at a consistently low level. Several measures can contribute to this goal over the next few months, while also allowing incremental increases in international travel:
- resurgence planning for a border-control failure and outbreaks of various sizes, with state-of-the-art contact tracing and an upgraded alert level system
- ensuring all New Zealanders own a re-useable fabric face mask with their use built into the alert level system
- conducting exercises and simulations to test outbreak management procedures, possibly including “mass masking days” to engage the public in the response
- carefully exploring processes to allow quarantine-free travel between jurisdictions free of COVID-19, notably various Pacific Islands, Tasmania and Taiwan (which may require digital tracking of arriving travellers for the first few weeks)
- planning for carefully managed inbound travel by key long-term visitor groups such as tertiary students who would generally still need managed quarantine.
Building back better
New Zealand cannot change the reality of the global COVID-19 pandemic. But it can leverage possible benefits.
We should conduct an official inquiry into the COVID-19 response so we learn everything we possibly can to improve our response capacity for future events.
We also need to establish a specialised national public health agency to manage serious threats to public health and provide critical mass to advance public health generally. Such an agency appears to have been a key factor in the success of Taiwan, which avoided a costly lockdown entirely.
Business as usual should not be an option for the recovery phase. A recent Massey University survey suggests seven out of ten New Zealanders support a green recovery approach.
New Zealand’s elimination of COVID-19 has drawn attention worldwide. We are about to publish an overview of the approach in the New England Journal of Medicine. We support a rejuvenated World Health Organization that could roll out an elimination model in other countries where there is public support for this approach.![]()
Michael Baker, Professor of Public Health, University of Otago; Amanda Kvalsvig, Senior Research Fellow, Department of Public Health, University of Otago, and Nick Wilson, Professor of Public Health, University of Otago
This article is republished from The Conversation under a Creative Commons license. Read the original article.





13 Comments
Pingback: บุหรี่นอกราคาถูก
Pingback: nagaway สล็อต
Pingback: ข่าวบอล
Pingback: คลินิกกายภาพบำบัด
Pingback: ความน่าเชื่อถือ Allbet Casino
Pingback: รับสร้างบ้านเชียงใหม่
Pingback: SWS Marketing
Pingback: ร้านเค้กวันเกิดใกล้ฉัน
Pingback: slot online เว็บนอก
Pingback: เค้กด่วน
Pingback: Aviation Tire
Pingback: ทัวร์ยุโรป
Pingback: 789bet